Air Quality
Dataset
Methodology
Residential greenness has been consistently associated with improved pregnancy outcomes and overall population health (Lee et al. 2020). Satellite-derived vegetation indices, particularly the Normalized Difference Vegetation Index (NDVI), are widely used as proxy measures of environmental quality and exposure to air pollution (Sedda et al. 2015). NDVI leverages the differential reflectance of vegetation in the visible red (RED) and near-infrared (NIR) spectral bands, with higher values indicating denser and healthier vegetation cover and, indirectly, lower levels of ambient air pollution.
Rationale
Satellite-derived vegetation indices, particularly NDVI, are widely used as proxy measures of environmental quality and exposure to air pollution. Higher values indicate denser and healthier vegetation cover. NDVI values range from -1 to 1, where values closer to 1 indicate dense, healthy vegetation.
References
Lee KJ, et al. (2020) Greenness, civil environment, and pregnancy outcomes. Environ Health 19:91. | Sedda L, et al. (2015) Poverty, health and satellite-derived vegetation indices. Int Health 7(2):99-106.
Dataset
Methodology
Residential proximity to major roadways is commonly used as a proxy for traffic-related air pollution exposure (Barnett et al. 2011). Epidemiological evidence indicates that women residing within proximity (e.g., ≤200m) to major roads experience an increased risk of adverse pregnancy outcomes, including preterm birth (Hitchins et al. 2000). Pollutants produced by motorized vehicles, such as carbon monoxide (CO), nitrogen oxide (NOx), hydrocarbons (HC), sulphur dioxide (SO2), lead (Pb) and carbon dioxide (CO2), have negative and dangerous impacts on the body (Rapang et al. 2023).
Rationale
Traffic-related pollutant concentrations exhibit a strong spatial gradient, with highest levels adjacent to roads and a non-linear decay with increasing distance. Exposure to vehicle emissions, particularly carbon monoxide (CO), during pregnancy has been identified as a potential factor contributing to low birth weight in infants.
References
Barnett AG, et al. (2011) Increased traffic exposure and negative birth outcomes. Environ Health 10:26. | Hitchins J, et al. (2000) Concentrations of submicrometre particles from vehicle emissions. Atmos Environ 34(1):51-9. | Rapang A, et al. (2023) Effect of CO exposure in pregnant women. J INFO Kesehat 21(4):713-20.
Dataset
Methodology
Population-weighted Euclidean distance to the nearest major road was computed using the same methodology as for highways, reflecting spatial variation in exposure to traffic-related pollution sources.
Dataset
Methodology
Elevation influences atmospheric pressure and air circulation patterns, which can affect the dispersion and concentration of air pollutants at a given location (Burton et al. 2025). Village-level altitude was derived by calculating the mean elevation pixel value within each village or neighbourhood boundary.
Rationale
In addition to affecting air pollutant dispersion, exposure to high-altitude environments has been associated with adverse reproductive and pregnancy outcomes, including low birth weight and increased risk of pregnancy complications (Burton et al. 2025).
References
Burton GJ, et al. (2025) Pregnancy at high altitude: the challenge of hypoxia. Phil Trans R Soc B 380(1933):20240167.
Dataset
Methodology
Air pollution is one of the top five health risk factors, contributing to 6.67 million deaths worldwide in 2019 (Zhong et al. 2025). Pregnant women and neonates with exposure to high levels of air pollutants are at increased risk of adverse health outcomes such as maternal hypertensive disorders, postpartum depression, placental abruption, low birth weight, preterm birth, infant mortality, and adverse lung and respiratory effects (Aguilera et al. 2023). Metrics were calculated by spatially averaging within a village's boundary.
Rationale
Exposure to fine particulate matter (PM2.5) has been associated with adverse maternal and birth outcomes, including increased risk of gestational hypertension and reduced birth weight (Makanga et al. 2019). Inhalation of ambient PM2.5 has been shown to cross the placenta and has been linked to adverse obstetric and postnatal metabolic health outcomes (Kaur et al. 2022).
References
Zhong K, et al. (2025) Susceptible window identification of maternal ozone exposure and preterm birth. Int Health. | Aguilera J, et al. (2023) Air pollution and pregnancy. Semin Perinatol 47(8):151838. | Kaur K, et al. (2022) PM2.5 exposure during pregnancy and placental lipid metabolic genes. Environ Res 211:113066.
Dataset
Rationale
Non-fire smoke PM2.5 represents background particulate matter from sources other than biomass burning, including industrial emissions, vehicle exhaust, and dust. This component contributes to chronic air pollution exposure during pregnancy.
Dataset
Rationale
Fire smoke PM2.5 captures particulate matter from biomass burning events including agricultural fires and wildfires. Seasonal burning patterns in sub-Saharan Africa can create acute exposure episodes during pregnancy.
Dataset
Rationale
Aerosol Optical Depth (AOD) is a measure of the extinction of solar radiation by aerosols in the atmospheric column. Higher values indicate greater atmospheric particle loading from all sources.
Dataset
Rationale
Dust AOD specifically captures desert dust aerosols. The Gambia's proximity to the Sahara Desert explains its higher dust loading compared to East African sites.
Dataset
Rationale
Black carbon aerosols originate primarily from incomplete combustion of fossil fuels and biomass burning. They contribute to respiratory and cardiovascular health impacts during pregnancy.
Dataset
Rationale
At a threshold of >2 ppm, CO was associated with lower mean birth-weight and higher rates of SGA and PTB, with a dose-response relationship (Galka et al. 2025). Acute CO poisoning in pregnant women is linked to complications such as preterm birth and miscarriage, with outcomes influenced by severity of maternal poisoning and stage of foetal development (Place et al. 2025). Exposure to vehicle emissions, particularly CO, during pregnancy has been identified as a potential factor contributing to low birth weight (Rapang et al. 2023).
References
Galka K, et al. (2025) Carbon monoxide levels and adverse pregnancy outcomes. Acta Obstet Gynecol Scand 104(12):2237-43. | Place E, et al. (2025) Carbon monoxide exposure in pregnant women in the UK. BMC Pregnancy Childbirth 25(1):1063.
Dataset
Rationale
Short-term exposure to NO2 may induce increased risk of Spontaneous Abortion (SAB) outpatient visits, especially in elder women and cool seasons (Liang et al. 2021).
References
Liang Z, et al. (2021) Short-term ambient nitrogen dioxide exposure is associated with increased risk of spontaneous abortion. Ecotoxicol Environ Saf 224:112633.
Dataset
Rationale
There is some positive correlation between Ozone (O3) and Preterm Birth which is mostly pronounced during middle pregnancy (Zhong et al. 2025).
References
Zhong K, et al. (2025) Susceptible window identification of maternal ozone exposure and preterm birth. Int Health ihaf073.
Dataset
Rationale
Sulfur dioxide (SO2) is a gaseous pollutant produced by fossil fuel combustion and volcanic activity. Exposure during pregnancy has been associated with respiratory symptoms and adverse birth outcomes.
Dataset
Methodology
Exposure to traffic-related pollution has been associated with increased risk of adverse pregnancy outcomes. Road density is commonly used as a spatial proxy for traffic intensity and associated vehicular emissions, with populations residing in communities with dense road networks experiencing higher exposure levels (Phillips et al. 2021).
References
Phillips BB, et al. (2021) Spatial extent of road pollution: A national analysis. Sci Total Environ 773:145589.
Spatial Access to Care
Dataset
Methodology
Road Quality Index (RQI) is derived from OpenStreetMap road network data combined with WorldPop gridded population estimates. The index quantifies the quality of road infrastructure accessible to residential populations by weighting road segments by their estimated speed limits.
Rationale
Road quality influences travel speed and accessibility to health facilities, with poorer road conditions associated with longer travel times and reduced access to maternal healthcare services. The quality of road infrastructure is a critical determinant of the "second delay" in maternal healthcare access - the delay in reaching an appropriate facility once the decision to seek care has been made (44).
Dataset
Methodology
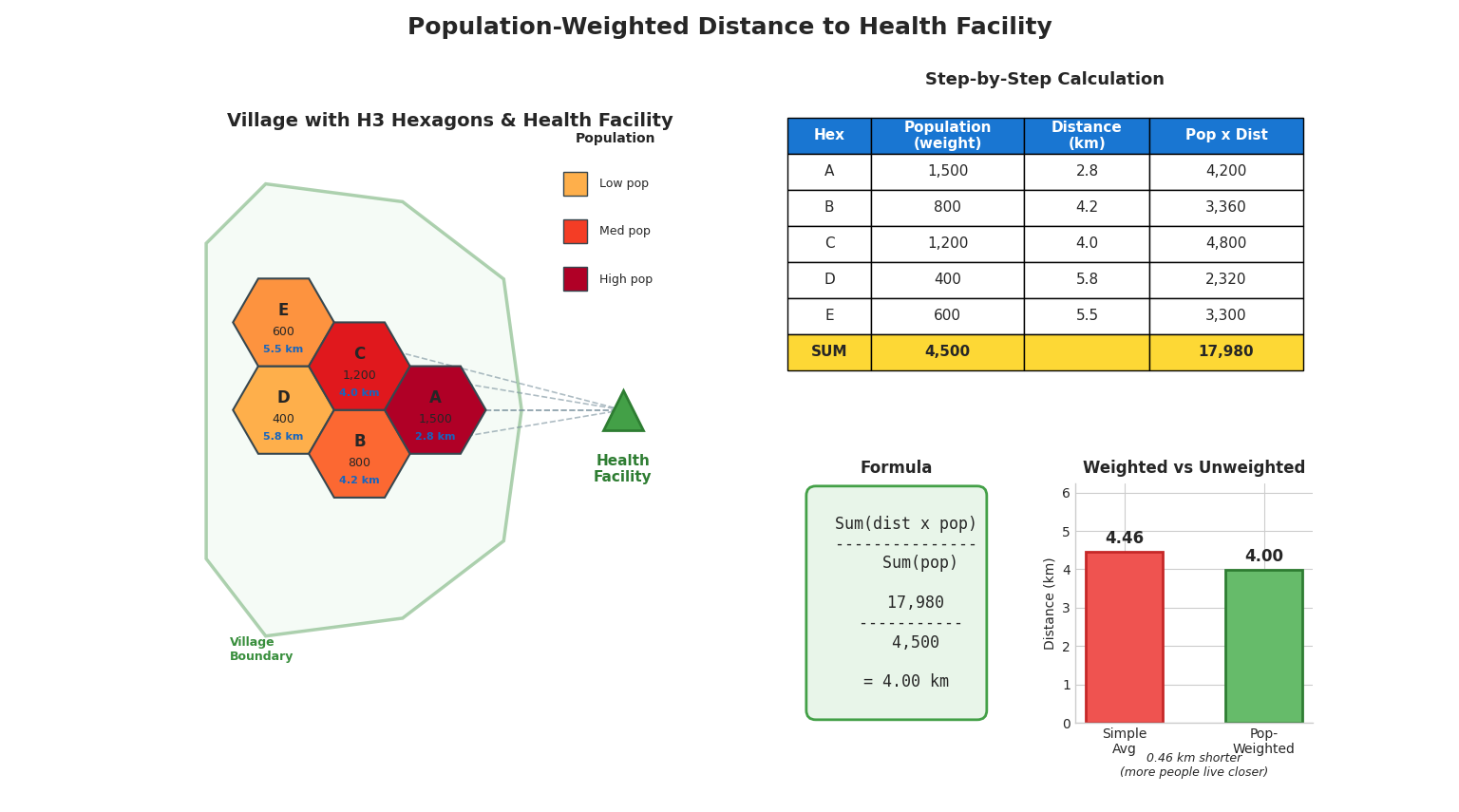
Population-weighted walking distance to the nearest health facility providing maternal healthcare services. Distances are computed using network routing algorithms that account for pedestrian pathways and terrain.
Rationale
Walking distance reflects accessibility for populations without motorized transport. In many sub-Saharan African settings, walking remains the primary mode of transport to health facilities, particularly for routine antenatal care visits (44).
Methodology
Walking time is derived from walking distance using a standard pedestrian walking speed assumption.
Rationale
Time-based accessibility metrics capture the temporal dimension of healthcare access. Walking times exceeding 60 minutes have been associated with reduced antenatal care utilization and increased risk of home delivery without skilled attendance (44).
Dataset
Methodology
Population-weighted driving distance to the nearest health facility using road network routing. Accounts for road network topology and driving restrictions.
Rationale
Driving distance represents motorized accessibility, which is critical for emergency obstetric care and referrals. Longer driving distances correlate with delays in reaching emergency care for obstetric complications (44).
Methodology
Driving time is computed using network routing algorithms that account for road type, speed limits, and traffic patterns.
Rationale
Travel time to nearest facility is a critical determinant of healthcare access. Delays reaching health facilities represent the "second delay" in Thaddeus and Maine's three-delays framework, which is known to elevate risks for adverse maternal outcomes (44).
Methodology
Public transport accessibility models a multi-modal journey combining walking to a pickup point on a main road and vehicle travel to the facility.
Rationale
Public transport represents the most common mode of motorized transport for pregnant women in resource-limited settings, particularly for planned antenatal visits. Accessibility via public transport captures the realistic journey patterns of women seeking maternal healthcare (44).
Methodology
Total public transport journey time combines walking, waiting, and in-vehicle components to model realistic travel patterns.
Rationale
Public transport journey times capture the full temporal burden of healthcare access, including waiting periods that disproportionately affect pregnant women. Journey times exceeding 2 hours are associated with reduced ANC attendance and delayed emergency care seeking (44).
Physical Isolation
Dataset
Methodology
Population-weighted walking distance to the nearest primary or secondary road, representing accessibility to major transport corridors.
Rationale
Walking distance to major roads is a proxy for isolation from transport networks. Difficult access to roads is a known barrier to healthcare utilization, particularly affecting women's ability to access public transport for antenatal care (4, 12).
Dataset
Methodology
Population-weighted walking distance to the nearest highway/trunk road, representing accessibility to national transport corridors.
Rationale
Walking distance to highways captures isolation from long-distance transport. Highways typically have inter-city bus services connecting to urban referral hospitals, which is critical for accessing higher-level emergency obstetric care (4, 12, 13).
Heat Exposure and Weather
Dataset
Methodology
Tier 1 is based on Wet-bulb temperature, extreme hot days and heatwave days. High temperature and humidity increase the risk of adverse pregnancy outcomes, while lower values are generally protective (Basu et al. 2010). Wet-bulb temperature integrates heat and humidity and is a physiologically relevant measure of maternal heat stress (Sherwood & Huber 2010).
Rationale
Wet bulb temperature is a superior heat stress metric as it accounts for the body's inability to cool through sweating in humid conditions. Values above 32°C are dangerous; above 35°C is lethal for prolonged exposure. Pregnant women are especially vulnerable to heat stress. Extreme hot days and heatwaves capture acute and sustained thermal stress beyond average conditions and have been linked to increased risks of preterm birth and stillbirth (McElroy et al. 2022).
References
Basu R, et al. (2010) High ambient temperature and risk of preterm delivery. Am J Epidemiol 172(10). | Sherwood SC, Huber M. (2010) An adaptability limit to climate change due to heat stress. PNAS 107(21):9552-5. | McElroy S, et al. (2022) Extreme heat, preterm birth, and stillbirth. Environ Int 158:106902.
Rationale
Percentage of pregnancy days exposed to extreme heat conditions. Extreme heat exposure during pregnancy affects fetal development through thermoregulatory stress and reduced placental blood flow.
Rationale
Prolonged heat exposure during heatwave events poses significant risks to maternal and fetal health. Heatwaves are defined as consecutive days exceeding the local 95th percentile temperature threshold.
Dataset
Methodology
Tier 2 is based on Ambient (2m) air temperature and Diurnal temperature. Ambient air temperature is used as an indicator of environmental heat exposure and has been associated with adverse pregnancy outcomes, with elevated temperatures increasing risk and lower temperatures showing protective effects (Basu et al. 2010).
Rationale
Low temperature and low humidity are protective against preterm birth, whereas high temperature increases risk. Evidence shows that estimated health effects are sensitive to the choice of temperature metric.
Methodology
Diurnal temperature variation reflects intra-day thermal instability rather than absolute heat exposure.
Rationale
Exposure to elevated diurnal temperature variation has been shown to be significantly associated with adverse early-life respiratory outcomes, including childhood pneumonia, indicating an independent exposure pathway related to repeated thermoregulatory stress (Xu et al. 2014).
References
Xu Z, et al. (2014) Temperature variability and childhood pneumonia. Environ Health 13:51.
Dataset
Methodology
Tier 3 is based on Land Surface Temperature (LST). LST represents the radiative temperature of the Earth's surface and is influenced by land cover, vegetation, and urban form.
Rationale
While LST does not directly represent ambient air temperature experienced by individuals, it provides valuable information on spatial heat patterns such as urban heat islands and localised heat accumulation, which shape pregnant women's exposure (Li & Bou-Zeid 2013).
References
Li D, Bou-Zeid E. (2013) Synergistic Interactions between Urban Heat Islands and Heat Waves. J Appl Meteorol Climatol 52(9):2051-64.
Precipitation
Dataset
Methodology
Monthly precipitation values were spatially averaged at the village or neighbourhood level.
Rationale
Seasonal variations in precipitation have been associated with fluctuations in birth outcomes, including birth weight and length (Rashid et al. 2017). Rainfall affects food availability, disease transmission, and access to healthcare during wet seasons.
References
Rashid H, et al. (2017) Temperature during pregnancy influences the fetal growth and birth size. Trop Med Health 45:1.
Relative Humidity
Dataset
Methodology
Rationale
Low relative humidity has been associated with reduced risk of preterm birth, whereas high relative humidity increases risk (Wu et al. 2023). Humidity affects thermal comfort, disease transmission, and food storage/safety.
References
Wu Y, et al. (2023) Effects of ambient temperature and relative humidity on preterm birth. Front Public Health 11:1101283.
Soil Micro-Nutrients
Dataset
Methodology
Values for each raster are averaged per neighbourhood/village boundary.
Rationale
Soil calcium affects food crop mineral content. Calcium is critical during pregnancy for fetal bone development, blood clotting, and muscle function. Maternal calcium deficiency is associated with preeclampsia and low birth weight.
Dataset
Rationale
Soil nitrogen is essential for plant protein synthesis and crop productivity. Low soil nitrogen contributes to food insecurity and maternal malnutrition.
Dataset
Rationale
Phosphorus is essential for root development and crop yield. Deficient soils produce lower crop yields affecting household food security.
Dataset
Rationale
Potassium regulates water uptake and disease resistance in plants, affecting agricultural productivity and food security.
Urban Form
Dataset
Methodology
Rationale
The ongoing urbanization worldwide is leading to an increasing number of pregnant women being exposed to higher levels of urban-related environmental hazards such as air pollution and noise, and at the same time, having less contact with natural environments. The urban environment during pregnancy may influence child's respiratory health (Li et al. 2025).
References
Li F, et al. (2025) The silent threat: effects of PM2.5 exposure on perinatal complications and neonatal outcomes. BMC Pregnancy Childbirth 25(1):686.
IPCC Climate Zone
Dataset
Methodology
Climate zones were assigned using the Intergovernmental Panel on Climate Change (IPCC) climate classification, based on long-term temperature and precipitation patterns (46). Village-level climate zones were determined using a population-weighted dominant classification.
Rationale
Climate zone classification provides contextual information relevant to environmental exposures during pregnancy, including thermal regimes and seasonal variability (47).
References
IPCC (2023) Climate Change 2021 – The Physical Science Basis. Cambridge University Press. | Watts N, et al. (2019) The 2019 report of The Lancet Countdown on health and climate change. Lancet 394(10211):1836-78.
Wealth and Development Indicators
Dataset
Methodology
VIIRS nighttime light intensity is widely used as a proxy for human settlement density, infrastructure development, and socioeconomic activity. Nighttime lights correlate strongly with population distribution, electrification, income, and access to services (Jean et al. 2016).
References
Jean N, et al. (2016) Combining satellite imagery and machine learning to predict poverty. Science 353(6301):790-4. | Chen X, Nordhaus WD. (2011) Using luminosity data as a proxy for economic statistics. PNAS 108(21):8589-94.
Dataset
Methodology
The Relative Wealth Index (RWI) is a high-resolution, machine-learning-derived proxy of relative household wealth developed by Meta Data for Good and validated against Demographic and Health Survey (DHS) wealth indices (Jean et al. 2016). RWI provides a continuous measure of socioeconomic status, with values interpreted relative to the national wealth distribution.
Rationale
Village-level socioeconomic context was estimated using a population-weighted RWI, accounting for within-village population distribution (Victora et al. 2008; Marmot et al. 2008).
References
Jean N, et al. (2016) Combining satellite imagery and machine learning to predict poverty. Science 353(6301):790-4. | Victora CG, et al. (2008) Maternal and child undernutrition. Lancet 371(9609):340-57. | Marmot M, et al. (2008) Closing the gap in a generation. Lancet 372(9650):1661-9.